6.4 Gas Exchange & Transport
Essential idea: The lungs are actively ventilated to ensure that gas exchange can occur passively.
Two processes maintain the concentration gradients between the blood and the alveolar air to ensure that diffusion of both oxygen and carbon dioxide can occur: firstly circulation of the blood brings a constant supply of high carbon dioxide, deoxygenated blood to the alveoli. Secondly the diaphragm (above) and intercostal muscles constantly increase and decrease the volume of the lungs to cause ventilation to occur, this is turn ensures a supply of high oxygen, low carbon dioxide air to the alveoli. The muscles cause the lungs to increase and decrease in volume by contractions. The striations help the muscle tissue to contract and relax.
Two processes maintain the concentration gradients between the blood and the alveolar air to ensure that diffusion of both oxygen and carbon dioxide can occur: firstly circulation of the blood brings a constant supply of high carbon dioxide, deoxygenated blood to the alveoli. Secondly the diaphragm (above) and intercostal muscles constantly increase and decrease the volume of the lungs to cause ventilation to occur, this is turn ensures a supply of high oxygen, low carbon dioxide air to the alveoli. The muscles cause the lungs to increase and decrease in volume by contractions. The striations help the muscle tissue to contract and relax.
Understandings:
6.4.U1 Ventilation maintains concentration gradients of oxygen and carbon dioxide between air in alveoli and blood flowing in adjacent capillaries.
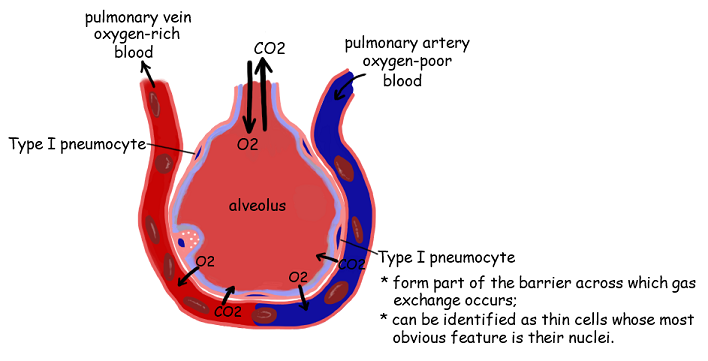
6.4.U2 Type I pneumocytes are extremely thin alveolar cells that are adapted to carry out gas exchange.
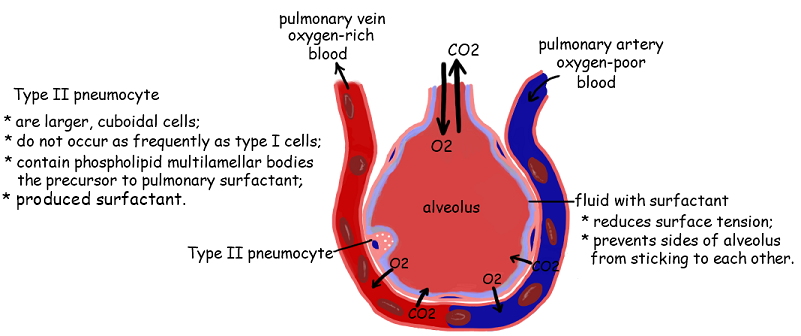
6.4.U3 Type II pneumocytes secrete a solution containing surfactant that creates a moist surface inside the alveoli to prevent the sides of the alveolus adhering to each other by reducing surface tension.
6.4.U4 Air is carried to the lungs in the trachea and bronchi and then to the alveoli in bronchioles. [Students should be able to draw a diagram to show the structure of an alveolus and an adjacent capillary.]
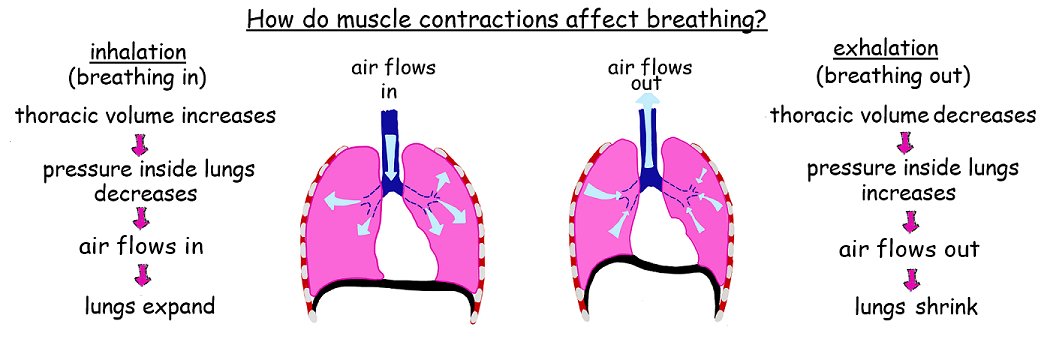
6.4.U5 Muscle contractions cause the pressure changes inside the thorax that force air in and out of the lungs to ventilate them.
6.4.U6 Different muscles are required for inspiration and expiration because muscles only do work when they contract.
Applications:
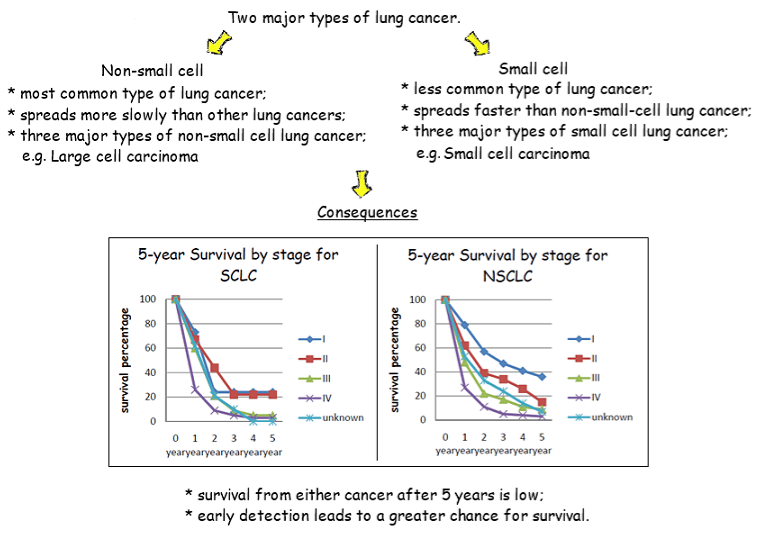
6.4.A1 Causes and consequences of lung cancer.
6.4.A2 Causes and consequences of emphysema.
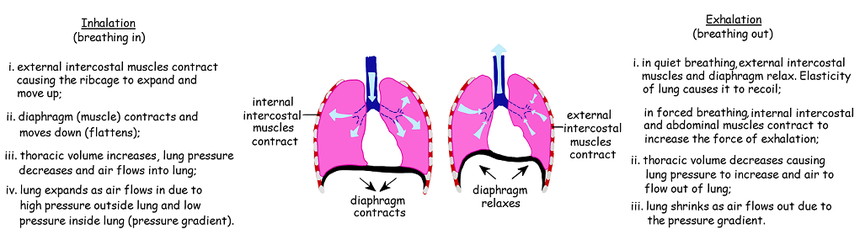
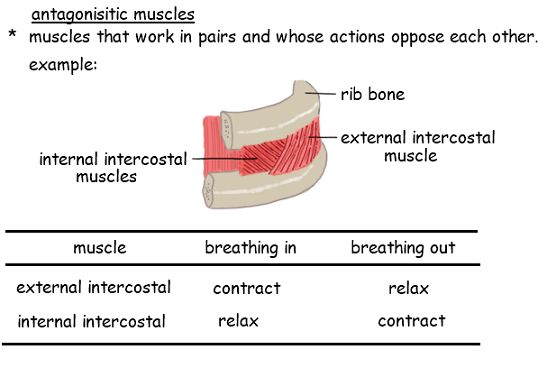
6.4.A3 External and internal intercostal muscles, and diaphragm and abdominal muscles as examples of antagonistic muscle action.
Skills:
6.4.S1 Monitoring of ventilation in humans at rest and after mild and vigorous exercise. (Practical 6) [Ventilation can either be monitored by simple observation and simple apparatus or by data logging with a spirometer or chest belt and pressure meter. Ventilation rate and tidal volume should be measured, but the terms vital capacity and residual volume are not expected.]
Nature of Science
Obtain evidence for theories—epidemiological studies have contributed to our understanding of the causes of lung cancer. (1.8)
6.4.U1 Ventilation maintains concentration gradients of oxygen and carbon dioxide between air in alveoli and blood flowing in adjacent capillaries.
6.4.U2 Type I pneumocytes are extremely thin alveolar cells that are adapted to carry out gas exchange.
6.4.U3 Type II pneumocytes secrete a solution containing surfactant that creates a moist surface inside the alveoli to prevent the sides of the alveolus adhering to each other by reducing surface tension.
6.4.U4 Air is carried to the lungs in the trachea and bronchi and then to the alveoli in bronchioles. [Students should be able to draw a diagram to show the structure of an alveolus and an adjacent capillary.]
6.4.U5 Muscle contractions cause the pressure changes inside the thorax that force air in and out of the lungs to ventilate them.
6.4.U6 Different muscles are required for inspiration and expiration because muscles only do work when they contract.
Applications:
6.4.A1 Causes and consequences of lung cancer.
6.4.A2 Causes and consequences of emphysema.
6.4.A3 External and internal intercostal muscles, and diaphragm and abdominal muscles as examples of antagonistic muscle action.
Skills:
6.4.S1 Monitoring of ventilation in humans at rest and after mild and vigorous exercise. (Practical 6) [Ventilation can either be monitored by simple observation and simple apparatus or by data logging with a spirometer or chest belt and pressure meter. Ventilation rate and tidal volume should be measured, but the terms vital capacity and residual volume are not expected.]
Nature of Science
Obtain evidence for theories—epidemiological studies have contributed to our understanding of the causes of lung cancer. (1.8)
6.4.U1 Ventilation maintains concentration gradients of oxygen and carbon dioxide between air in alveoli and blood flowing in adjacent capillaries.
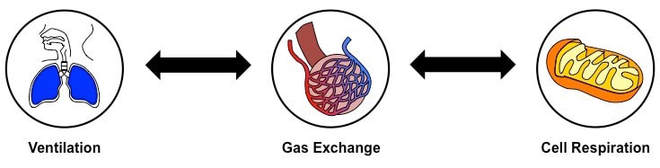
Physiological respiration involves the transport of oxygen to cells within the tissues, where energy production occurs.
The processes involved in physiological respiration are:
Physiological respiration involves the transport of oxygen to cells within the tissues, where energy production occurs.
The processes involved in physiological respiration are:
- Ventilation: The exchange of air between the atmosphere and the lungs – achieved by the physical act of breathing
- Gas Exchange: The exchange of oxygen and carbon dioxide between the alveoli and bloodstream (via passive diffusion)
- Cell Respiration: The release of energy (ATP) from organic molecules – it is enhanced by the presence of oxygen (aerobic)
Purpose of Ventilation
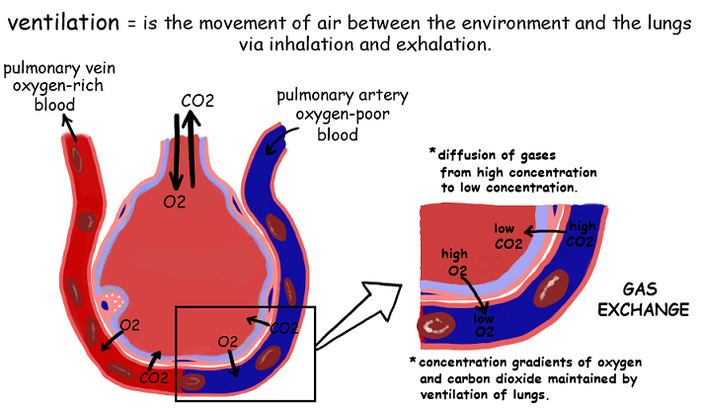
Because gas exchange is a passive process, a ventilation system is needed to maintain a concentration gradient in alveoli
Because gas exchange is a passive process, a ventilation system is needed to maintain a concentration gradient in alveoli
- Oxygen is consumed by cells during cellular respiration and carbon dioxide is produced as a waste product
- This means O2 is constantly being removed from the alveoli into the bloodstream (and CO2 is continually being released)
- This means O2 levels stay high in alveoli (and diffuse into the blood) and CO2 levels stay low (and diffuse from the blood)
- The lungs are also structured to have a very large surface area, so as to increase the overall rate of gas exchange
6.4.U2 Type I pneumocytes are extremely thin alveolar cells that are adapted to carry out gas exchange.
The Respiratory System
Structure of an Alveolus
Alveoli function as the site of gas exchange, and hence have specialised structural features to help fulfil this role:
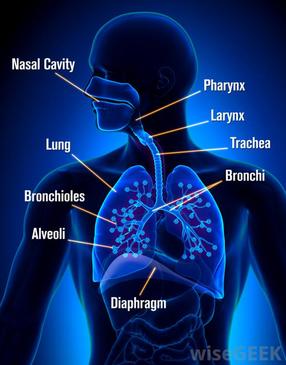
- Air enters the respiratory system through the nose or mouth and passes through the pharynx to the trachea
- The air travels down the trachea until it divides into two bronchi (singular: bronchus) which connect to the lungs
- The right lung is composed of three lobes, while the left lung is only comprised of two (smaller due to position of heart)
- Inside each lung, the bronchi divide into many smaller airways called bronchioles, greatly increasing surface area
- Each bronchiole terminates with a cluster of air sacs called alveoli, where gas exchange with the bloodstream occurs
Structure of an Alveolus
Alveoli function as the site of gas exchange, and hence have specialised structural features to help fulfil this role:
- They have a very thin epithelial layer (one cell thick) to minimise diffusion distances for respiratory gases
- They are surrounded by a rich capillary network to increase the capacity for gas exchange with the blood
- They are roughly spherical in shape, in order to maximise the available surface area for gas exchange
- Their internal surface is covered with a layer of fluid, as dissolved gases are better able to diffuse into the bloodstream
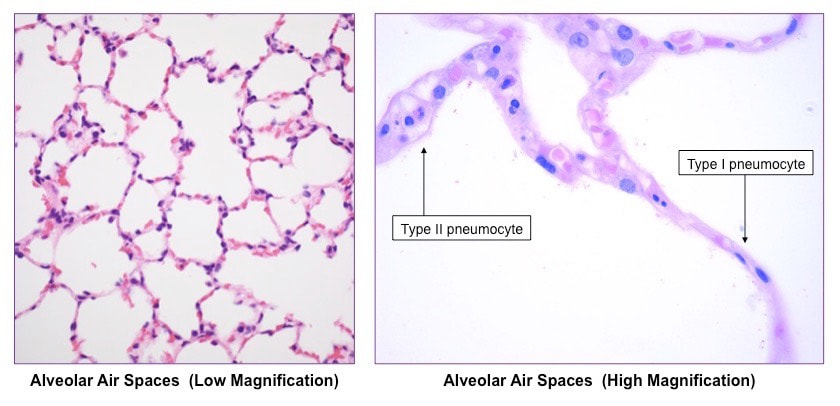
Pneumocytes (or alveolar cells) are the cells that line the alveoli and comprise of the majority of the inner surface of the lungs
Type I pneumocytes
- There are two types of alveolar cells – type I pneumocytes and type II pneumocytes
Type I pneumocytes
- Type I pneumocytes are involved in the process of gas exchange between the alveoli and the capillaries
- They are squamous (flattened) in shape and extremely thin (~ 0.15µm) – minimising diffusion distance for respiratory gases
- Type I pneumocytes are connected by occluding junctions, which prevents the leakage of tissue fluid into the alveolar air space
- Type I pneumocytes are amitotic and unable to replicate, however type II cells can differentiate into type I cells if required
6.2.U3 Type II pneumocytes secrete a solution containing surfactant that creates a moist surface of the alveoli to prevent the sides of the alveolus adhering to each other by reducing surface tensions
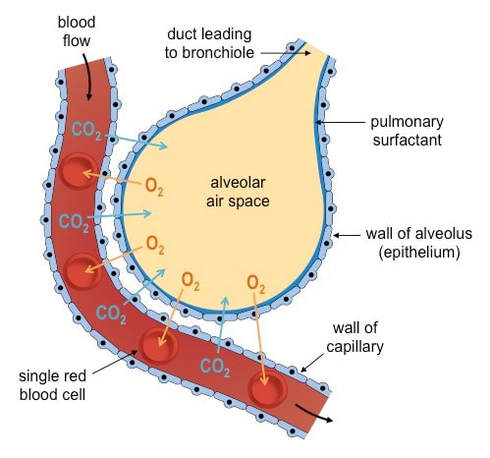
Alveoli are lined by a layer of liquid in order to create a moist surface conducive to gas exchange with the capillaries
Alveoli are lined by a layer of liquid in order to create a moist surface conducive to gas exchange with the capillaries
- It is easier for oxygen to diffuse across the alveolar and capillary membranes when dissolved in liquid
- About 5% of the inner surface of the alveoli consists of Type II pneumocytes
- These cells secrete a liquid made of proteins and lipids called surfactant
- This liquid allows oxygen to dissolve into the surfactant and then diffuse into the blood
- It also provides a medium for carbon dioxide to evaporate into the air inside the alveoli in order to be exhaled
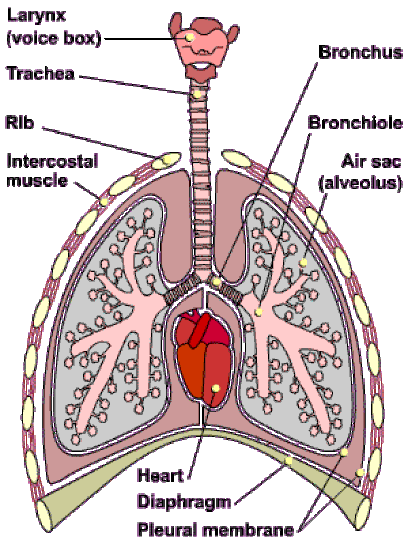
Cross section of the lung
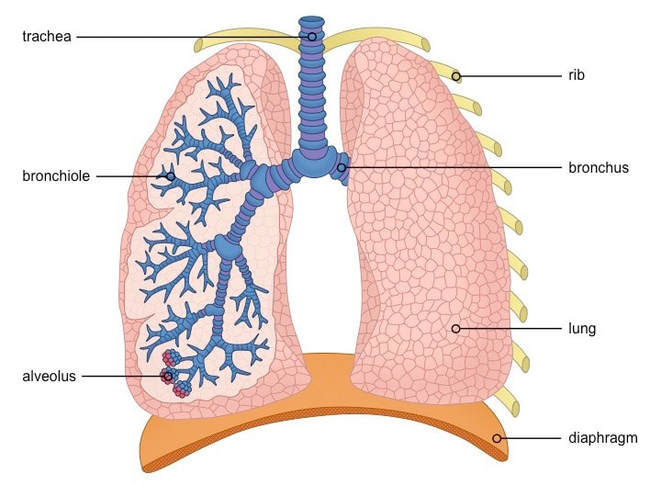
6.4.U5 Air is carried to the lungs in the trachea and bronchi and then to the alveoli in bronchioles.
- Air enters the respiratory system through the nose or mouth and travels through the pharynx and then the trachea (made from rings of cartilage)
- The trachea divides into two bronchi (left and right)
- Inside each lung the bronchi divide into many smaller tubes called bronchioles
- These numerous bronchioles form a tree root-like structure that spreads throughout the lungs
- Each bronchiole ends in a cluster of air sacs called alveoli
6.2.U5 Muscle contractions cause the pressure changes inside the thorax that force air in and out of the lungs to ventilate them
Gases will move from a region of high pressure to a region of lower pressure (similar to movement via concentration gradient)
Gases will move from a region of high pressure to a region of lower pressure (similar to movement via concentration gradient)
- When the pressure in the chest is less than the atmospheric pressure, air will move into the lungs (inspiration)
- When the pressure in the chest is greater than the atmospheric pressure, air will move out of the lungs (expiration)
6.2.U6 Different muscles are required for inspiration and expiration because muscles only do work when they contract
Applications
6.2.A1 Causes and consequences of lung cancer
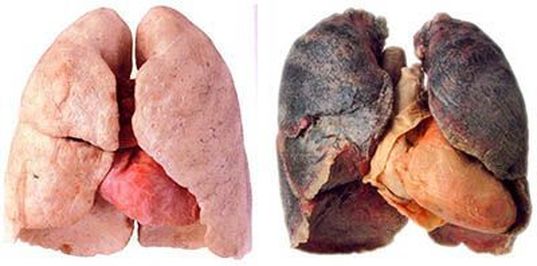
Lung cancer describes the uncontrolled proliferation of lung cells, leading to the abnormal growth of lung tissue (tumour) The abnormal growth can impact on normal tissue function, leading to a variety of symptoms according to size and location The tumours can remain in place (benign) or spread to other regions of the body (malignant)
Lung cancers are the most common cause of cancer-related death worldwide for two main reasons: The lungs are vital to normal body function and thus the abrogation of their normal function is particularly detrimental to health The lungs possess a very rich blood supply, increasing the likelihood of the cancer spreading (metastasis) to other body regions
The common symptoms of lung cancers include coughing up blood, wheezing, respiratory distress and weight loss If the cancer mass compresses adjacent organs it can cause chest pain, difficulty swallowing and heart complications
The common symptoms of lung cancers include coughing up blood, wheezing, respiratory distress and weight loss If the cancer mass compresses adjacent organs it can cause chest pain, difficulty swallowing and heart complications
Common Risk Factors for Lung Cancer
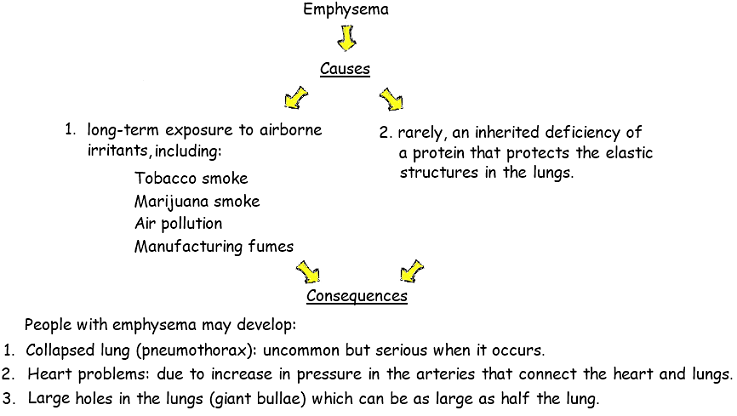
6.2.A2 Causes and consequences of emphysema
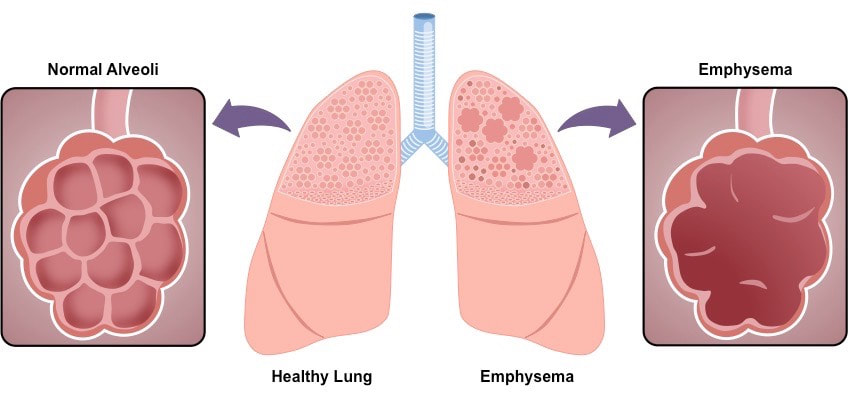
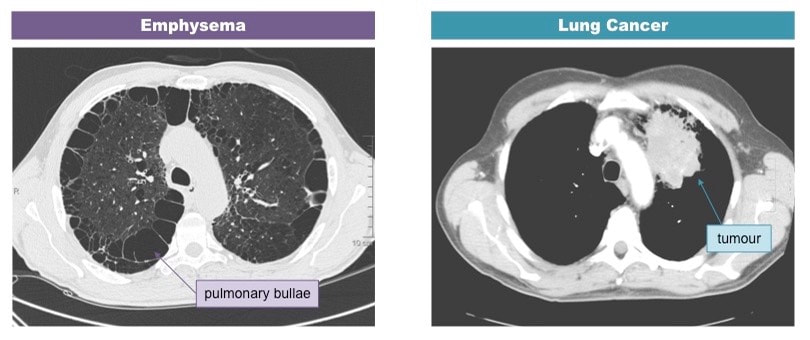
Emphysema is a lung condition whereby the walls of the alveoli lose their elasticity due to damage to the alveolar walls The loss of elasticity results in the abnormal enlargement of the alveoli, leading to a lower total surface area for gas exchange The degradation of the alveolar walls can cause holes to develop and alveoli to merge into huge air spaces (pulmonary bullae)
Visualisation of Lung Disorders Using CT Scanning
6.2.A3 External and internal intercostal muscles, and diaphragm and abdominal muscles are examples of antagonistic muscle action
Skills
6.1.S1 Monitoring of ventilation in humans at rest and after mild and vigorous exercise
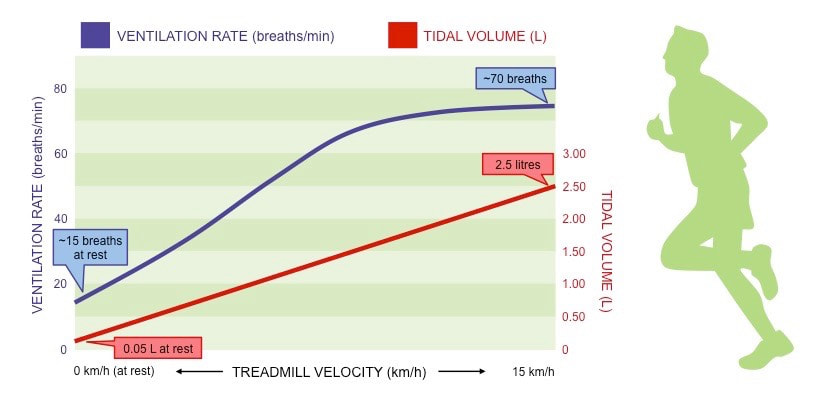
Ventilation in humans changes in response to levels of physical activity, as the body’s energy demands are increased
Trends in Tidal Volume and Breathing Frequency
6.1.S1 Monitoring of ventilation in humans at rest and after mild and vigorous exercise
Ventilation in humans changes in response to levels of physical activity, as the body’s energy demands are increased
- ATP production (via cellular respiration) produces carbon dioxide as a waste product (and may consume oxygen aerobically)
- Changes in blood CO2 levels are detected by chemosensors in the walls of the arteries which send signals to the brainstem
- As exercise intensity increases, so does the demand for gas exchange, leading to an increase in levels of ventilation
- Increase ventilation rate (a greater frequency of breaths allows for a more continuous exchange of gases)
- Increase tidal volume (increasing the volume of air taken in and out per breath allows for more air in the lungs to be exchanged)
Trends in Tidal Volume and Breathing Frequency
Measuring Ventilation
Ventilation in humans can be monitored in a number of ways:
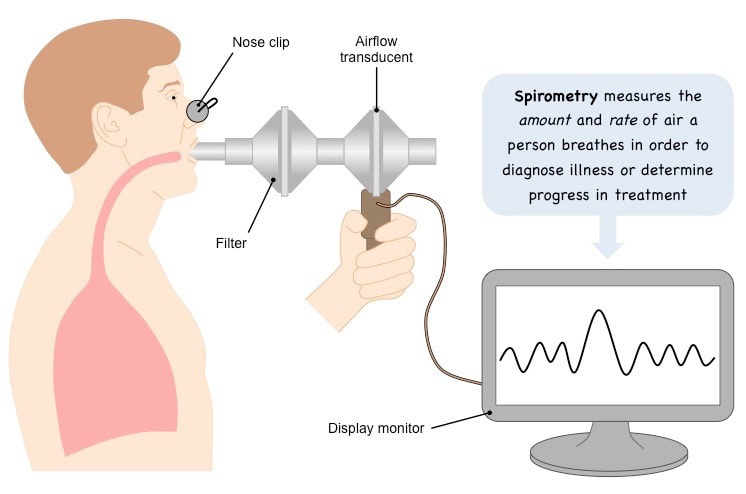
Measuring Ventilation with a Spirometer
Ventilation in humans can be monitored in a number of ways:
- Via simple observation (counting number of breaths per minute)
- Chest belt and pressure meter (recording the rise and fall of the chest)
- Spirometer (recording the volume of gas expelled per breath)
- A spirometer is a device that detects the changes in ventilation and presents the data on a digital display
- A more simplistic method involves breathing into a balloon and measuring the volume of air in a single breath
- The volume of air can be determined by submerging the balloon in water and measuring the volume displaced (1ml = 1cm3)
Measuring Ventilation with a Spirometer